
Microbiology lab manuals, increasingly utilizing open educational resources, bridge theoretical knowledge with practical application, aiding diagnosis of infectious diseases and student comprehension.
Importance of Microbiology Labs in Education
Microbiology laboratories are pivotal in education, transforming theoretical concepts into tangible skills. They foster critical thinking, problem-solving, and meticulous technique – essential for future scientists and healthcare professionals. The increasing adoption of open educational resources (OERs) makes quality lab experiences more accessible.
Practical application, as found in a comprehensive lab manual, reinforces understanding of microbial worlds. Students learn aseptic techniques, staining procedures, and culturing methods, directly relating to disease diagnosis. These hands-on experiences are crucial, especially considering the clinical relevance emphasized in modern microbiology education, preparing students for real-world challenges.
Overview of a Microbiology Lab Manual
A comprehensive microbiology lab manual serves as a student’s guide, detailing procedures and safety protocols. Modern manuals, like the Leboffe Microbiology Lab Manual, aim for user-friendliness, assisting with product understanding and functionality. They often emphasize the clinical laboratory’s role in diagnosing infectious diseases, bridging theory and practice.
These manuals typically cover essential topics: aseptic techniques, staining, culturing, and identification methods. They may also include sections on molecular techniques and immunological methods. A well-structured manual, potentially utilizing OERs, provides clear instructions, safety guidelines, and preparatory information, even accounting for right-handed users, ensuring a successful lab experience.

Essential Lab Equipment and Techniques
Microbiology labs require specialized tools – microscopes, sterilization equipment – and precise techniques for safe handling of microbial cultures and accurate analysis.
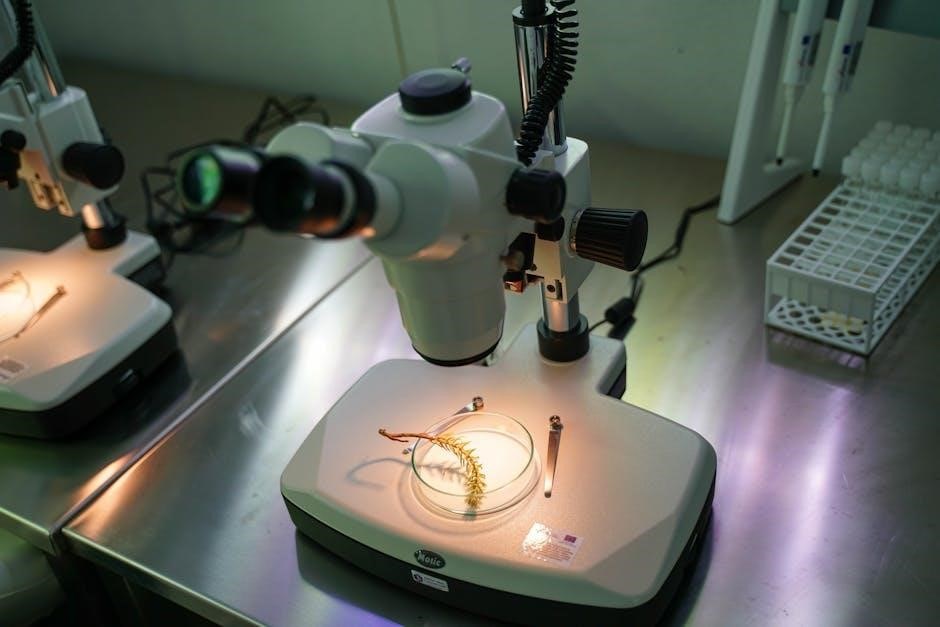
Microscopes and Their Applications
Microscopes are fundamental tools in microbiology, enabling visualization of microorganisms beyond the resolution of the naked eye. Brightfield microscopy, the most common type, provides a direct image, while techniques like phase contrast enhance contrast for unstained specimens.
Understanding magnification and resolution is crucial; magnification increases apparent size, while resolution determines the level of detail visible. Different objective lenses offer varying magnification powers.
Beyond basic observation, microscopy aids in morphological identification – determining cell shape, size, and arrangement. Specialized staining techniques, coupled with microscopy, reveal internal structures and aid in classification. The small size of microbes necessitates careful microscopic examination for accurate analysis and diagnosis.
Sterilization and Disinfection Methods
Sterilization and disinfection are critical for maintaining a pure culture and preventing contamination in microbiology labs. Sterilization, the complete elimination of all microbial life, is typically achieved through autoclaving – using high-pressure steam. Other methods include dry heat sterilization and filtration.
Disinfection, conversely, reduces the number of microorganisms but doesn’t necessarily eliminate all. Common disinfectants include alcohol, bleach, and phenolic compounds. The choice of disinfectant depends on the target microorganisms and the surface being treated.
Proper handling and disposal of biohazardous materials, alongside adherence to established safety guidelines, are paramount. These procedures ensure a safe working environment and reliable experimental results.
Culture Media Preparation and Types
Culture media provide the nutrients necessary to support microbial growth in vitro. Preparation involves dissolving dehydrated media components in distilled water, adjusting pH, and sterilizing, typically by autoclaving. Media types are diverse, categorized by consistency, chemical composition, and functional use.
Broth media are liquid, supporting large-scale growth. Agar media are solid, enabling isolation of pure cultures. Defined media have known compositions, while complex media contain undefined components like yeast extract.
Selective media inhibit unwanted organisms, and differential media distinguish between different microbial groups based on metabolic characteristics. Careful media selection is crucial for successful microbial cultivation.
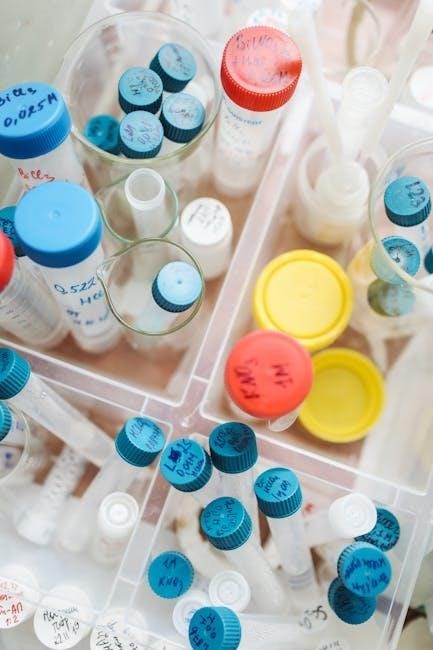
Basic Microbiological Techniques
Microbiological techniques, essential for safe handling, include aseptic transfer, staining for visualization, and diverse culturing methods for isolating and studying microbes.
Aseptic Techniques and Their Significance
Aseptic technique is paramount in microbiology, preventing contamination of cultures, personnel, and the environment. This involves sterilizing equipment, disinfecting work surfaces, and employing careful handling procedures during inoculation and transfer.
The small size of microorganisms necessitates strict adherence to these protocols. Contamination can lead to inaccurate results, misidentification of organisms, and potentially hazardous exposures. Proper technique minimizes unwanted microbial growth, ensuring reliable experimental outcomes.
Manuals emphasize the importance of these practices, often detailing step-by-step procedures for maintaining a sterile field. Right-handed individuals will find instructions tailored accordingly, highlighting the precision required for successful microbiological work.
Bacterial Staining Methods (Gram Stain, Acid-Fast Stain)
Bacterial staining is a fundamental technique in microbiology, enhancing visualization of cellular morphology and aiding in identification. The Gram stain differentiates bacteria based on cell wall structure – Gram-positive retaining crystal violet, Gram-negative appearing pink after counterstaining.
The acid-fast stain, crucial for identifying Mycobacterium species, utilizes carbolfuchsin to stain cells with mycolic acid in their walls, resisting decolorization with acid-alcohol. These methods, detailed in lab manuals, are essential for clinical diagnosis.
Understanding staining principles and proper execution are vital, as accurate interpretation relies on correct procedure and microscopic examination. These techniques provide critical initial data for further biochemical testing.
Culturing Techniques: Streak Plate, Pour Plate, Spread Plate
Microbial culturing is central to microbiology, enabling isolation and growth of microorganisms. The streak plate method dilutes a sample across an agar surface, yielding isolated colonies. Pour plate techniques involve mixing a sample with molten agar before plating, resulting in colonies within and on the agar.
Spread plate methods distribute a diluted sample across the agar surface, promoting surface colony formation. These techniques, detailed in lab manuals, require aseptic technique to prevent contamination.
Choosing the appropriate method depends on the desired outcome – isolation of pure cultures versus estimating viable cell counts. Proper execution ensures accurate representation of the original sample.

Identification of Microorganisms
Microorganism identification relies on biochemical tests, microscopic examination, and dichotomous keys, crucial for accurate diagnosis and detailed lab manual application.
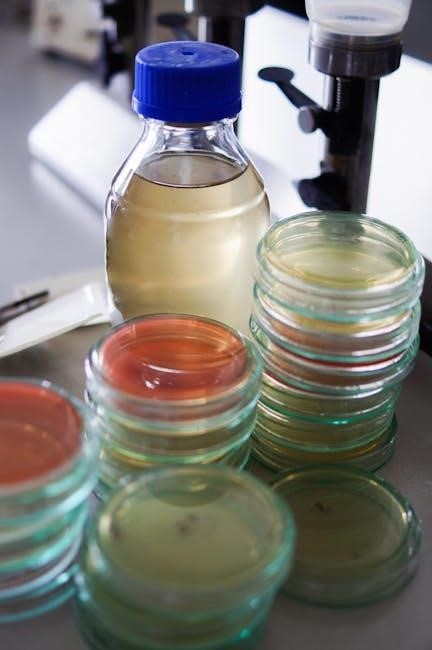
Biochemical Tests for Bacterial Identification
Biochemical tests are fundamental in identifying bacteria, exploiting their metabolic differences. These tests assess a bacterium’s ability to utilize specific substrates or produce particular enzymes. Common examples include catalase, oxidase, and various fermentation tests – like sugar fermentation – revealing acid or gas production.
The clinical microbiology laboratory heavily relies on these tests for accurate diagnosis of infectious diseases. Manuals detail protocols for each test, emphasizing proper controls and interpretation of results. Understanding these metabolic pathways is crucial, linking theoretical knowledge to practical application. Accurate identification guides appropriate antibiotic therapy and infection control measures, directly impacting patient care.
Microscopic Examination of Fungi and Parasites
Microscopic examination is vital for identifying fungi and parasites, differing significantly from bacterial identification. Fungal structures like hyphae and spores require specific staining techniques – such as lactophenol cotton blue – for clear visualization. Parasites, often larger and more complex, necessitate careful observation of morphology and motility.
Lab manuals detail preparation methods for direct smears and specialized stains. Accurate identification relies on recognizing characteristic features; for example, identifying Candida species or parasitic eggs. This skill is crucial in clinical settings, aiding in the diagnosis of mycoses and parasitic infections. Understanding these microscopic features links theory to practical application, impacting patient treatment.
Using Dichotomous Keys for Identification
Dichotomous keys are essential tools in microbiology labs for systematically identifying microorganisms. These keys present a series of paired, mutually exclusive statements, forcing users to choose between two options at each step. This process progressively narrows down possibilities based on observed characteristics.
Lab manuals emphasize the importance of accurate observation when utilizing these keys. Correct identification hinges on precisely noting morphological traits and biochemical test results. While often used for bacteria, dichotomous keys can also aid in fungal and parasitic identification. Mastering this skill reinforces the link between theoretical knowledge and practical application, crucial for accurate diagnoses.

Applications in Clinical Microbiology
Clinical microbiology labs diagnose infectious diseases through specimen analysis – urine, blood, and more – alongside antibiotic susceptibility testing procedures.
Specimen Collection and Handling
Proper specimen collection is paramount in clinical microbiology, directly impacting accurate diagnoses. Protocols must minimize contamination and ensure representative samples are obtained from the infection site. This involves selecting appropriate collection devices – swabs, fluids, tissues – and employing correct techniques based on the suspected pathogen.
Handling procedures are equally critical. Specimens require prompt transport to the lab, often with specific temperature controls to preserve viability. Accurate labeling with patient details and collection date/time is essential. Detailed documentation of the collection process, including any observed characteristics, aids in interpretation. Following standardized procedures guarantees reliable results and patient care.
Analysis of Urine, Blood, and Other Clinical Samples
Clinical microbiology labs perform diverse analyses on patient samples. Urine analysis detects urinary tract infections via microscopy, culture, and biochemical tests. Blood cultures identify bloodstream infections, requiring stringent aseptic technique to avoid contamination. Other samples – wound swabs, cerebrospinal fluid, sputum – undergo similar processing.
Analysis techniques include direct microscopic examination for immediate pathogen identification, followed by culture to grow and isolate organisms. Biochemical tests characterize bacterial species, while molecular methods like PCR offer rapid, specific detection. Accurate interpretation requires correlating lab findings with clinical presentation for effective patient management.
Antibiotic Susceptibility Testing
Antibiotic susceptibility testing (AST) is crucial for guiding effective treatment of bacterial infections. Methods include disk diffusion (Kirby-Bauer), broth microdilution, and E-tests, determining the minimum inhibitory concentration (MIC) of various antibiotics against a specific isolate.
Interpretation follows Clinical and Laboratory Standards Institute (CLSI) guidelines, categorizing results as susceptible, intermediate, or resistant. AST informs clinicians about appropriate antibiotic choices, combating antimicrobial resistance. Accurate AST requires standardized procedures, quality control, and careful documentation to ensure reliable patient care and responsible antibiotic stewardship.

Advanced Techniques and Emerging Trends
Molecular techniques like PCR and DNA sequencing, alongside immunological methods, are revolutionizing microbiology labs and enhancing disease surveillance capabilities.
Molecular Microbiology Techniques (PCR, DNA Sequencing)
Molecular microbiology represents a paradigm shift in diagnostic capabilities. Polymerase Chain Reaction (PCR) allows for rapid amplification of specific DNA sequences, enabling swift pathogen detection even in low concentrations. This technique is invaluable for identifying infectious agents and genetic markers associated with antibiotic resistance.
Furthermore, DNA sequencing provides a detailed genetic fingerprint of microorganisms, crucial for outbreak investigations and understanding evolutionary relationships. These advanced methods complement traditional culture-based techniques, offering increased sensitivity and specificity. The integration of these technologies into clinical microbiology labs is transforming infectious disease management, facilitating personalized medicine and proactive public health strategies.
Immunological Methods in Microbiology
Immunological techniques are pivotal in detecting microbial antigens and antibodies, offering rapid and specific identification. Serological assays, like ELISA and agglutination tests, detect antibody-antigen interactions, aiding in diagnosing current or past infections. These methods are particularly useful when direct microbial detection is challenging.
Immunofluorescence assays utilize fluorescently labeled antibodies to visualize microbial antigens directly within clinical samples. Furthermore, flow cytometry allows for the quantification of immune cell populations and their response to microbial stimuli. These techniques are essential for understanding host-pathogen interactions and developing effective vaccines and immunotherapies, enhancing diagnostic precision in microbiology labs.
The Role of Microbiology Labs in Disease Surveillance
Microbiology laboratories are central to public health, actively participating in disease surveillance networks. They identify and characterize pathogens, tracking outbreaks and monitoring antimicrobial resistance patterns. Accurate and timely reporting of infectious disease data to public health agencies is crucial for informed decision-making.
Labs contribute to early warning systems, detecting emerging infectious diseases and novel strains. Molecular techniques, like PCR and DNA sequencing, enable rapid pathogen identification and genomic analysis, facilitating outbreak investigations. Continuous surveillance informs preventative measures, guiding vaccination campaigns and antibiotic stewardship programs, ultimately protecting community health and minimizing disease impact.
Safety Considerations in the Microbiology Lab
Microbiology labs demand strict adherence to biosafety levels, proper biohazardous material handling, and established emergency protocols to protect personnel and the environment.
Biosafety Levels and Practices
Microbiology laboratories operate under a tiered biosafety level (BSL) system, ranging from BSL-1 (basic teaching labs) to BSL-4 (handling dangerous and exotic agents). Each level dictates specific containment practices and safety equipment.
BSL-1 requires standard microbiological practices, like handwashing and disinfection. BSL-2 adds limited access, biohazard warning signs, and sharps precautions. Higher levels—BSL-3 and BSL-4—demand specialized facilities, personnel training, and stringent protocols, including respiratory protection and controlled access zones.
Essential practices across all levels include proper waste disposal, decontamination of work surfaces, and reporting of accidents. Manuals emphasize these guidelines, ensuring a safe learning and research environment. Adherence minimizes risks associated with handling potentially infectious materials.

Handling and Disposal of Biohazardous Materials
Microbiology labs generate biohazardous waste – cultures, stocks, contaminated materials – requiring careful handling and disposal. Proper segregation is crucial; sharps (needles, slides) go into puncture-resistant containers, while liquids and solids are autoclaved or chemically disinfected before disposal.
Biohazard bags, clearly labeled, are used for contaminated solid waste. Manuals detail specific procedures for each waste type, adhering to local regulations. Spill kits are essential for immediate cleanup of accidental releases, preventing further contamination.
Personnel must be trained in these protocols, understanding the risks and proper procedures. Safe handling minimizes exposure and protects both lab workers and the environment, ensuring responsible laboratory practice.
Emergency Procedures in the Microbiology Lab
Microbiology labs necessitate well-defined emergency protocols. These include procedures for spills (biohazardous materials, chemicals), exposures (skin contact, inhalation, ingestion), and fires. Every lab must prominently display emergency contact information and evacuation plans.
Spill kits, readily accessible, contain materials for safe containment and cleanup. Exposure protocols detail immediate first aid – washing affected areas, seeking medical attention – and reporting procedures. Fire drills should be conducted regularly to ensure familiarity with evacuation routes.
Comprehensive lab manuals outline these procedures, emphasizing swift and appropriate response to minimize harm and prevent further contamination. Regular training is vital for all personnel.